Priorisation and optimisation of multimedication in elderly multimorbid patients in general practice
![]() Project content
Project content
PRIMUM - PRIorisation of MUltimedication in Multimorbid patients.
A study sponsored by the German Federal Ministry for Education and Research (BMBF).
The provision of medical care to chronically ill patients is one of the central challenges facing developed industrial countries. Taken within the context of a demographic shift in the population, the problems of co- and multimorbidity and the multimedication that is generally associated with them are increasingly prevalent. Multimedication - that is taking five or more medicines at the same time - is associated with substantial risk, such as of drug interactions and / or unwanted adverse events (UAE), resulting in hospitalization and higher mortality rates. Furthermore, multimedication is often accompanied by reduced therapy adherence.
International studies have shown that amongst other methods electronic warning systems, by generating a warning signal, are a suitable means of avoiding potentially inappropriate prescriptions. However, current evidence is insufficient: up to now interventions have only been concerned with individual phases of the medication process. In addition, randomised controlled studies in the German family practice setting are lacking.
On the basis of evidence from international studies, a method to optimise medication prescriptions was developed that targets the whole medication process. In order to relieve the burden on family doctors, the contribution that can be made by certified health care assistants in the practice are also considered in the study.
![]() Intervention concept
Intervention concept
Identify medication-related problems by means of a checklist (Medication-Monitoring-List, MediMoL) in a preparatory interview with the healthcare assistant
Utilise the internet-based medication information service (AiD Arzneimittelinformations-Dienst)
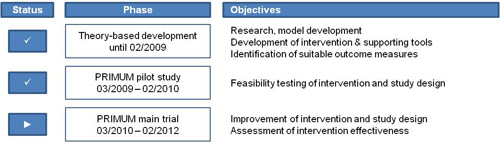
Family doctor consults the patient with regard to medication related problems The method that, consisting of several components, is also known as a complex intervention, is currently undergoing a step-by-step analysis:
![]() Sponsors
Sponsors
The project is being conducted independently of industry funding and is being sponsored by the German Federal Ministry for Education and Research (BMBF, support code: 01GK0702).
![]() Team
Team
- Dr. med. Christiane Muth, MPH (Principal Investigator)
- Undergraduate Assistants: Stephanie Braun, Christina Conrad, Christian Diaz-Florez, Mariam Shila Hassan, Anja Päsel, Julia Ruhland, Maike Schmidt, Nuray Tetik
![]() Cooperation partners
Cooperation partners
- Prof. Dr. med. Walter Emil Haefeli,
Clinical Pharmacology & Pharmacoepidemiology, University Hospital, Heidelberg [link] - Prof. Dr. med. Sebastian Harder,
Institute of Clinical Pharmacology / ZAFES, Johann Wolfgang Goethe University Hospital, Frankfurt am Main [link] - Dipl.-Psych. Justine Rochon, M.Sc.,
Institute for Medical Biometry and Informatics (IMBI), University Hospital, Heidelberg [link] - Prof. Dr. Frank Oswald,
Interdisciplinary Gerontology, Institute for Social Pedagogy and Adult Education, Goethe University, Frankfurt am Main [link]
![]() Scientific Advisory Board
Scientific Advisory Board
- Prof. André Knottnerus und Marjan van den Akker, PhD
Netherlands School of Primary Care Research - CaRe, Department of General Practice, Maastricht University [link] - Rafael Pereira, DPhil
Centre for Evidence Based Medicine, Department of Primary Health Care, University of Oxford [link] - Jose M Valderas, MD, PhD, MPH
NIHR School of Primary Care Research, Division of Public Health and Primary Health Care, University of Oxford [link]
![]() Practice Advisory Board
Practice Advisory Board
- Dr. med. Joachim Fessler (Flörsheim), Dr. med. Alexander Liesenfeld (Amöneburg-Mardorf), Dr. med. Joachim Seffrin (Weiterstadt)
- Karola Mergenthal, Vera Müller (both from the Institute for General Practice, Johann Wolfgang Goethe University Frankfurt)
- Pre-pilot phase: Prof. Dr. med., Dipl.-Päd. Jochen Gensichen, MPH,
Institute of General Practice, Friedrich Schiller University / University Hospital, Jena [link]
